magazine_ Article
How altitude can impact neurological conditions
Recommendations for climbing at altitude
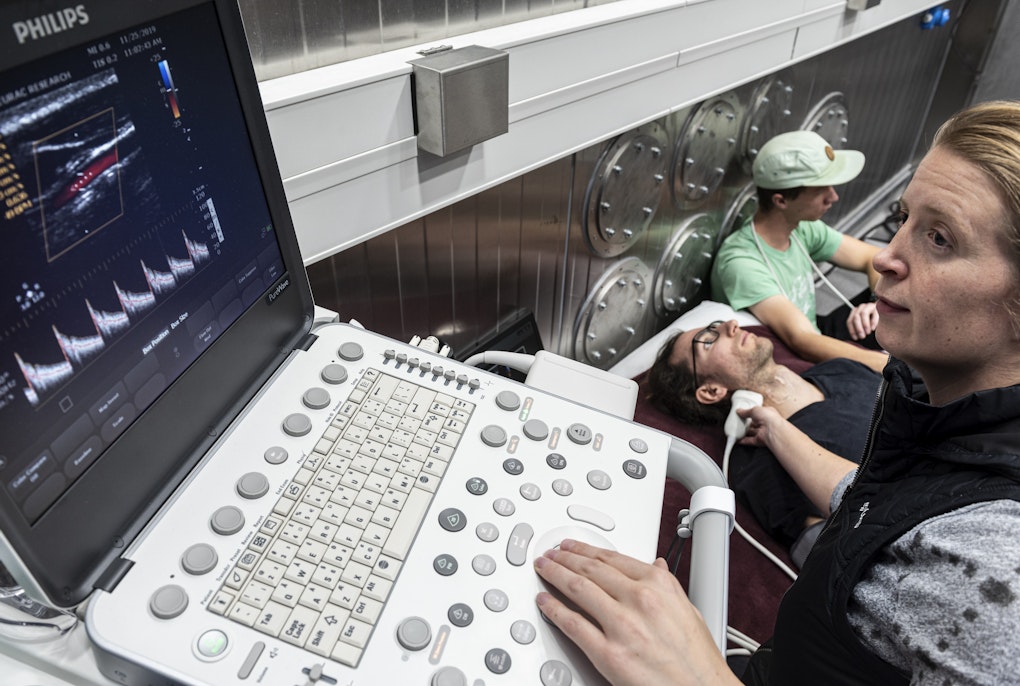
A research team from Eurac Research, the Universities of Trento and Padua and the Hospital of Aosta assessed the risks of exposure to high altitude for a variety of neurological conditions from migraine to Parkinson's and multiple sclerosis to stroke.
Steven (not his real name) is in his tent at an altitude of 4,250 meters, in the middle of a mountaineering expedition, when he is suddenly seized by convulsions. Steven is young, physically fit, and well acclimatized. Doctors rule out a form of acute mountain sickness as the cause. Only later do they discover that his family has a history of epilepsy, although prior to the expedition, he had never experienced any epileptic episodes.
“From anything higher than about 2,000 metres, altitude can have various effects on the nervous system. The body’s first reaction to oxygen deprivation is to increase cerebral perfusion, enabling more blood to reach the brain. This is normal, but under certain conditions it can cause problems,” explains Marika Falla, neurologist and researcher at Eurac Research and the University of Trento. “Those who travel to altitude without the necessary acclimatization risk developing varying degrees of serious high-altitude disorders – from acute mountain sickness to cerebral oedema. Those who do so with overt or latent neurological disorders should be even more cautious, and in some cases should avoid going to higher altitudes all together”.
Steven’s is just one of the many examples that Falla and her colleagues Corrado Angelini from the University of Padua and Guido Giardini from Aosta Hospital, encountered during their research, the results of which were recently published in the Journal of Central Nervous System Disease. After analyzing data from clinical studies and dozens of cases reported from the 1970s to the present day, the group outlined the precautions to be taken by those with neurological conditions interested in high-altitude excursions.
There are headaches. And there are Headaches
Eighty percent of people who live at low altitudes experience a condition known as 'altitude headache’ when climbing above 3,000 meters. About 12 percent of the world’s population experience migraines, with peaks of up to 25 percent among women of childbearing age; headaches are probably the most common neurological disorder. But what happens if a person prone to migraines climbs to high altitudes? According to the research team, it is difficult for non-specialists to distinguish a habitual migraine attack from headaches caused by altitude or headaches associated with acute mountain sickness, especially if they are not accompanied by other symptoms such as nausea, poor appetite or vomiting, fatigue and dizziness. However, the fact is that migraine attacks tend to increase at altitude, but not to the extent that hiking is not recommended. “A migraine patient planning a trek or an expedition at altitude should bring along the medication usually taken to control attacks and make sure to climb gradually. High altitude is not recommended, however, if the person is undergoing a period of frequent migraines,” explains Falla.
A special case however is a migraine with atypical aura. If you have been diagnosed with this type of migraine, you should carefully consider any high-altitude excursions and consult with a doctor. Acute cases may in fact require sudden investigations and that may be complicated, especially in remote areas - quite common when you are at high altitude.
Depression is another one of the latent disorders that can manifest at altitude. The conditions of stress and isolation experienced during certain mountaineering expeditions, combined with environmental conditions that affect the neurochemical balance can accentuate mood swings. Unfortunately, the drugs most used for such conditions – such as benzodiazepines – are strongly discouraged at altitude.
People who have had a stroke in the previous 90 days should avoid at all costs climbing at altitude because even if they feel well, their neurological situation is unstable.
When no means no
The scientific article does not mention whether Steven was able to climb his summit as planned, but if he were a keen mountaineer, he would probably have a few more expeditions on his CV today. Fortunately, epilepsy – like migraines and the mild cognitive impairments suffered by many elderly people – is not incompatible with altitude if it is stabilized properly with therapy. According to Falla and her colleagues, the cases in which climbing at altitude should be avoided at all costs are limited to people who have had a stroke in the previous 90 days because even if they feel well, their neurological situation is unstable. In addition, people with diabetic neuropathy, brain tumors and advanced neuromuscular diseases should also avoid excursions at altitude because a lack of oxygen would put their already compromised respiratory muscles under additional stress. “People with diabetic neuropathy, which affects the peripheral nervous system, have sensory disturbances in their extremities, which can result in a situation in which they cannot ‘feel’ their feet, so walking for long periods on rough terrain, especially in unsuitable clothing such as tight shoes, can contribute to the appearance of injuries and aggravate pre-existing damage,” explains Falla. “For tumors, on the other hand, the problem is that atmospheric pressure as well as lack of oxygen, alter blood pressure and cerebral blood flow . The balance between the components of the nervous system is altered and if there is a tumor mass pressing on the brain structures, this altered balance might increase and the tumor mass pressing on brain structures may provoke symptoms. It is no coincidence that the first signs of a brain tumor can sometimes appear at altitude”.
| Absolute contraindications to high altitude excursions | Unstable conditions, such as having experienced a stroke in the past 90 days |
| Diabetic neuropathy | |
| Brain tumors | |
| Neuromuscular diseases accompanied with severe respiratory impairment | |
| Relative contraindications to high altitude excursions Each case should be assessed by a neurologist with specific experience |
Epilepsy stabilized with the therapy |
| Parkinson’s disease and mild cognitive impairment which could be associated with sleep apnea syndrome or not | |
| Migraine |
Parkinson patients
In our increasingly ageing societies, neurodegenerative diseases such as Parkinson’s, which affects around 1 percent of over 60s, are increasing. In the advanced stages, people are unfortunately no longer autonomous, but up to a certain point they may wish to travel or go on organized trips. Indeed, physical activity is recommended to stimulate the body and fight depression. "Each case should be assessed by an expert, to avoid some conditions getting worse, but also to avoid unjustified bans and thus plan your trips in the best possible way," says Falla. There is no specific data on how Parkinson patients react at high altitude, but what we know about the disease helps to draw conclusions. "For example, many Parkinson patients suffer from sleep apnea. The combination of hypoxia and apnea could cause breathing difficulties, but, if the general picture allows, this could be overcome by limiting oneself to daily trips to high altitude and returning to sleep in the valley". A key recommendation: never venture alone in the mountains. But, this also applies to everyone, even if you don’t have a neurological condition.