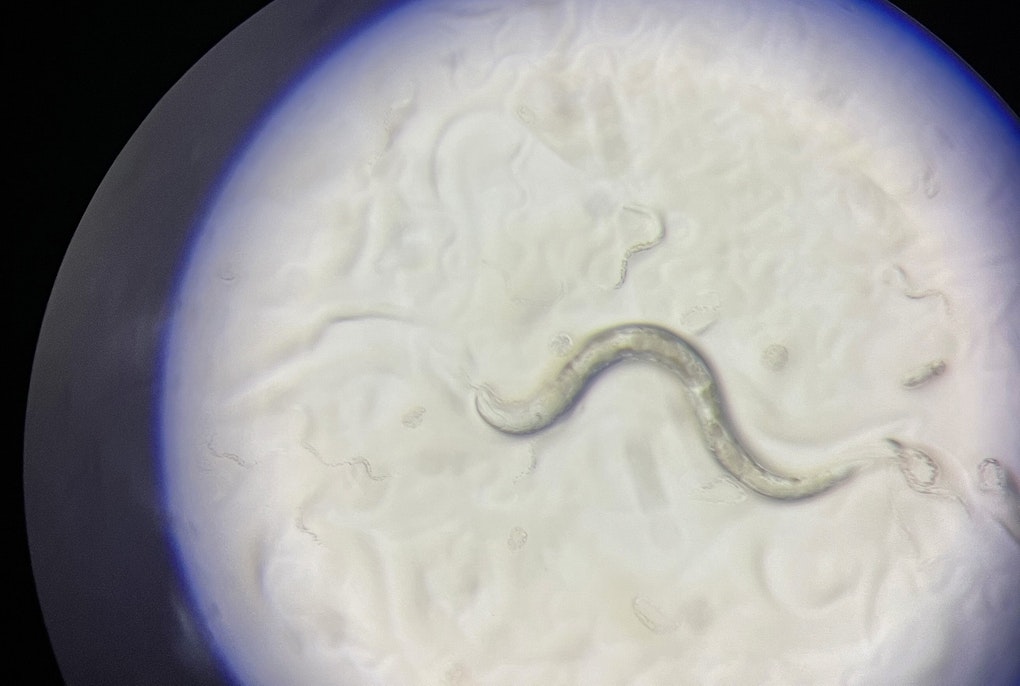
In 2011, scientists at the University of Pisa proved that Francesco I de' Medici, Grand Duke of Tuscany (shown here in a portrait by Scipione Pulzone), died of malaria by analyzing his skeleton. Now a research team led by Eurac Research has detected the pathogen of the dangerous malaria tropica in soft tissue from embalming vessels - but in this case it is unknown from which family member the tissue originated.
Photo: Scipione Pulzone - public domain | All rights reserved
magazine_ Article
Malaria in the Medici era
The pathogen of the deadliest form of the disease has been identified in mummified soft tissue belonging to members of the Florentine dynasty.
Malaria was common in Renaissance Italy. The disease was known as “Febbre terzana” at the time as an onset of the fever occurred in intervals of two to three days. A research team led by Eurac Research has now microscopically detected the parasite Plasmodium falciparum, the causative agent of the dangerous malaria tropica in soft tissue from embalming vessels found at the Basilica di San Lorenzo in Florence.
The powerful dynasty buried its dead according to a special ritual: during embalming, the entrails were removed and placed in large terracotta vessels called orci which were buried together with the coffins in the Basilica di San Lorenzo in Florence. In 2010, researchers were allowed to sample nine of these orci which were decorated with the family’s coat-of-arms. Of the nine, two bore the names of specific family members. Using long tweezers, the team retrieved something that at first glance seemed to Anthropologist Albert Zink who was leading the investigation, to be “rather insignificant,”. He went on to explain, “However, these fragments, which to the untrained eye, could have been pieces of cloth, were in fact mummified tissues of unknown origin. So, our first interest was to find out what we were actually looking at. Then, to find out if the structure of the organ was intact enough to see if we could identify the organ it came from.” The researchers took a total of 24 samples, which they then subjected to microscopic and molecular analyses.
The molecular investigations did not lead much further. The material was too degraded, the Arno had flooded Florence several times since the Medici period and acute temperature fluctuations had done the rest, “proteins or DNA were almost no longer present,” explains first author of the study, Microbiologist Frank Maixner. “But it wasn’t all bad news, the microscopic structure was in fact, very exciting.” Thin tissue sections revealed a potential blood vessel that still contained collections of red blood cells. When a special method called Giemsa staining was used, evidence of a parasite inside these blood cells was revealed. What Maixner described “a surprising finding” was not conclusive. The parasites could have been plasmodia – a parasite responsible for malaria or even another parasite called babesia.
The team went on to employ an even more precise technique, atomic force microscopy whereby the tissue surface was scanned with a nanoscopic needle which rendered even the tiniest differences in height and three-dimensional structure visible. This analysis revealed the typical ring-shaped structures that characterize one of the developmental stages of the plasmodia parasites. However, the same shapes can also be formed by babesia
An even more precise technique was used, atomic force microscopy: surfaces are scanned with a nanoscopically fine needle, making even the tiniest differences in height and three-dimensional structures visible. And indeed, the typical ring-shaped structures that characterize one of the developmental stages of the plasmodia parasites - but which can also be formed by babesia - could be seen.
Finally, it was the immunohistochemical method, which enables the detection of antigens in tissue sections, that provided certainty. And so, the parasite was determined unambiguously: Plasmodium falciparum, the causative agent of the deadliest form of malaria, malaria tropica, which occurs mainly in the equatorial region.
Parasites were detected in many of the blood cells examined. In addition, typical membrane structures formed by the Plasmodium falciparum pathogen itself during the course of infection could be detected within the individual blood cells. “These so-called Maurer's clefts are cell organelles that are important for interaction between host and parasite. Among other things, they are involved in the transport of parasite proteins and as such significantly influence the course of the disease” explains co-author and Malaria Researcher Nicole Kilian from the University of Heidelberg/University Hospital Heidelberg.
In a further analysis, the scientists examined the sugar structures on the surface of the blood cells, which decisively influence blood group. The result: the infected individual belonged to blood group B and, people from this blood group are less resistant to malaria. However, it is no longer possible to find out which family member the results pertain as the orci from which the sample was taken does not bear a name.
 technical documentation
technical documentationThe Study
The study, which involved research institutions from Europe, the United States and Korea, appeared in the June issue of the journal Emerging Infectious Diseases can be found here: https://wwwnc.cdc.gov/eid/article/29/6/23-0134_article