magazine_ Article
Cardiac arrest: investigating causes
A heart disease common in young people is being researched at the cellular level
A young athlete suddenly collapses in the middle of the sports field. The rescue team is unable to bring the young person back to life and can only determine cardiac arrest as cause of death. Cases like this are reported again and again and raise the question of how such a tragedy could happen so abruptly. One of the most common causes of sudden cardiac death in young people is hypertrophic cardiomyopathy, a congenital genetic disorder that affects one in 500. The underlying mechanisms are currently being investigated in the HYPER-FIBRO project.
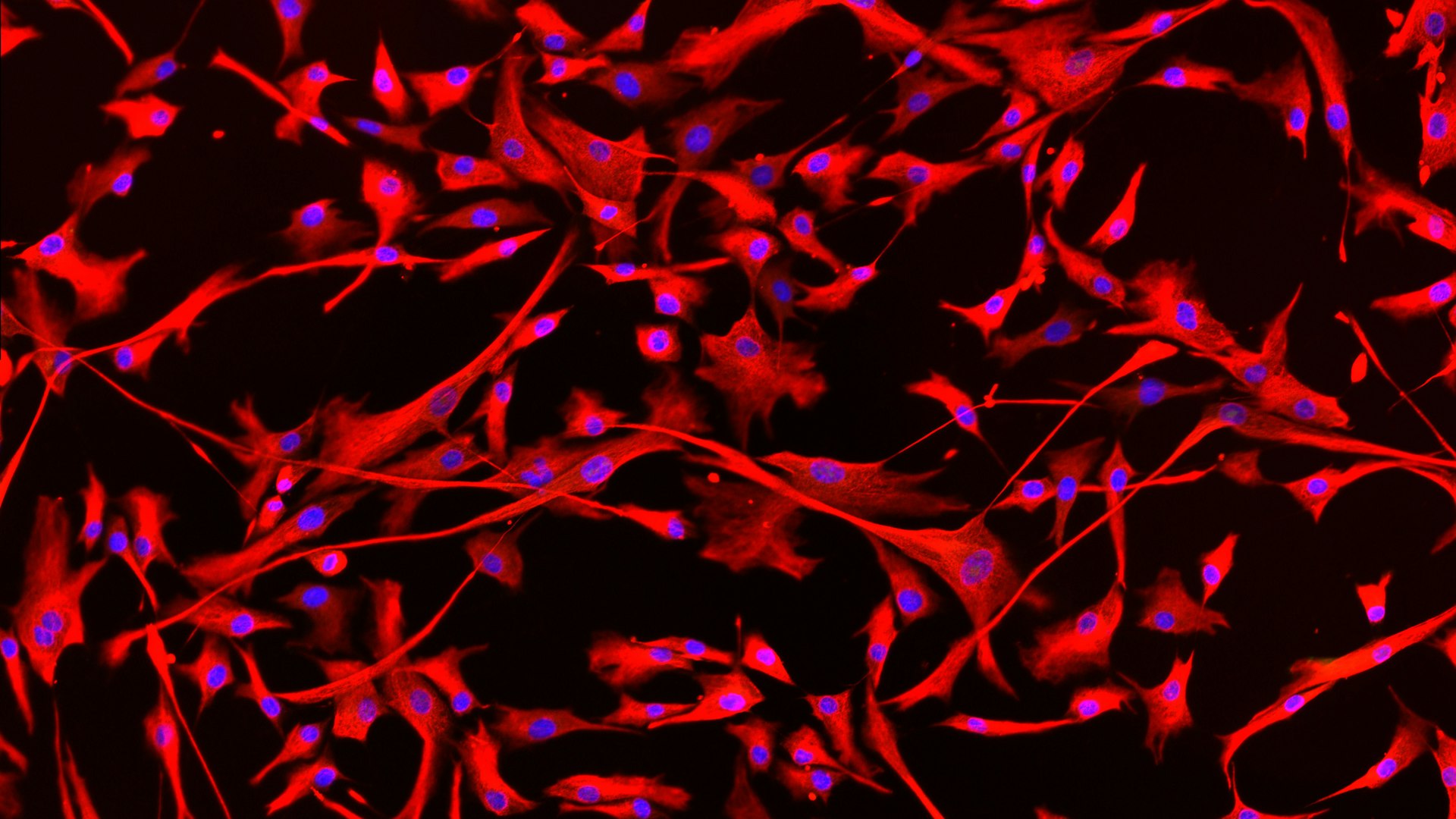
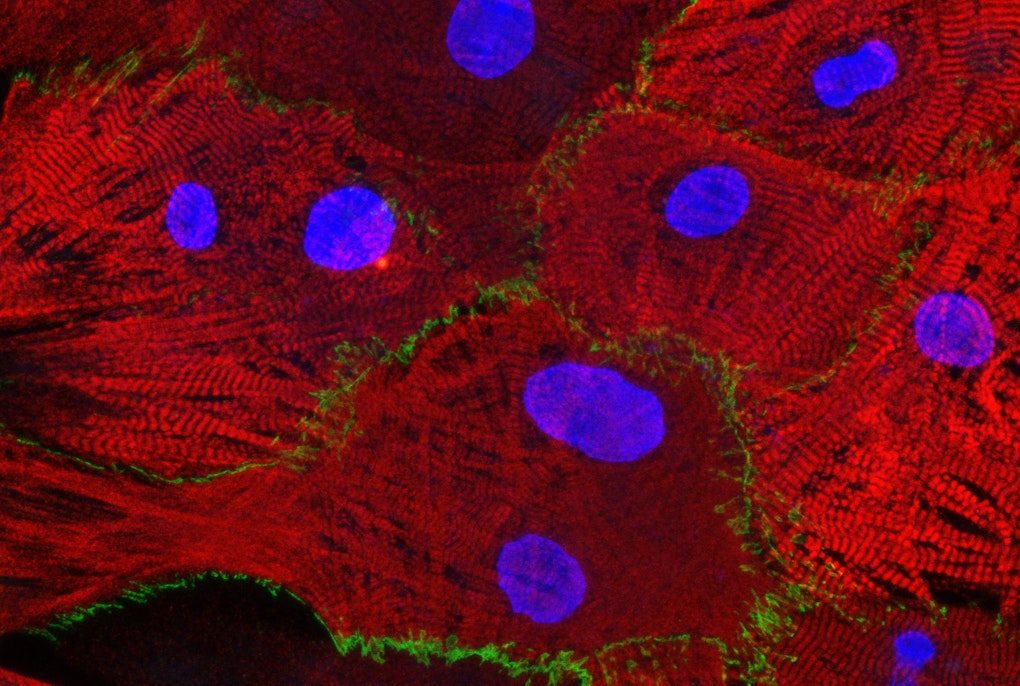
At Eurac Research's Institute of Biomedicine, molecular biologist Maja Schlittler studies how the heart cells of patients with hypertrophic cardiomyopathy (HCM) behave. "Cardiomyopathy" is the term used to describe a pathological change in the heart muscle, and the "hypertrophic" part stands for the excessive growth of the cells which cause the heart wall to thicken visibly. When the disease manifests, the heart muscle cells grow in an uncontrolled manner. In addition, the heart forms an excess of scar tissue, also known as "fibrosis". "Cells that produce fibrotic tissue are called fibroblasts and so far, no one has investigated their role in HCM, although excessive fibrosis is a well-recognized potential cause of malignant arrhythmias," Schlittler explains. "Normally, connective tissue cells form a network that supports the structure of the heart. When there is an injury in the heart, the connective tissue cells migrate there and 'patch' it up, forming the scar tissue," Schlittler clarifies. "In diseased patients however, it can happen that the connective tissue cells become highly activated, and the scar tissue becomes too thick." This thickening can lead to disturbances in heartbeat: The electrical signal is no longer transmitted properly, and because the heart wall is too thick, there may be problems ejecting blood. In the course of the disease, shortness of breath and cardiac arrhythmias can occur, leading to sudden cardiac death in the worst case.
If drug treatment does not stop the pathological growth of the heart cells, the excess tissue is surgically removed. Maja Schlittler works with small samples of this tissue, provided by the group of Prof. Elisabetta Cerbai, at the University of Firenze. From the small fragments, she amplifies cardiac fibroblasts and observes their behavior under certain stimuli. In the HYPER-FIBRO research project, she wants to understand why too many fibroblasts are produced in patients with HCM and how certain active substances affect their growth.
To do this, Schlittler used tissue samples from five HCM patients in order to examine various properties of the fibroblasts, namely their size, shape and ability to proliferate and move around in the culture dish. She also added a fluorescent marker to the cells to see exactly which of the cells were activated and so potentially able to form scar tissue.
The next step is now to investigate both molecularly and functionally why the cardiac fibroblasts of HCM patients form so much scar tissue compared to healthy cardiac fibroblasts.
Schlittler hopes to provide a basis for new therapeutic approaches for HCM based on her investigation. "Our results will feed into international biomedical research and help to better understand the causes of this heart disease and which agents could be used to treat it," says Schlittler.
The project was funded by an International Mobility grant of the Autonomous Province of Bolzano.
About the Interviewed
Maja Schlittler grew up in Switzerland. After her studies at ETH Zurich, she worked in the field of clinical research both in Switzerland and Australia. She did her PhD at the Karolinska Institutet in Stockholm on "Molecular adaptations of skeletal muscle in health and disease". Since 2020, she has been working in the "Biology of Cardiac Health and Disease" research group under the supervision of Alessandra Rossini at Eurac Research’s Institute of Biomedicine.